 Book Now
Book Now
2 Ahmed Elmlihy St. from Venny Square, Dokki, Giza, Egypt

Home | Services | In Vitro Fertilization (IVF)
Released at:Dec, 27 2023 •

As the leading IVF center in Egypt, we understand the challenges of infertility and are dedicated to helping you navigate your path to parenthood. IVF, a widely recognized Assisted Reproductive Technology (ART), has emerged as an effective solution to diverse fertility issues when other treatments may not be suitable.
The IVF journey begins with the surgical extraction of the female patient's eggs through an oocyte retrieval procedure. These eggs can be utilized immediately, known as a fresh cycle, or cryopreserved for future use. Freezing eggs or embryos can serve a host of personal reasons, such as planning for future parenthood or preserving fertility. When the time is right, the frozen eggs or embryos are thawed, marking the commencement of a frozen cycle.
To facilitate fertilization, the male partner is asked to provide a sperm sample on the day of egg collection or from a pre-frozen sample at our clinic. In the secure confines of our state-of-the-art laboratory, the extracted eggs and sperm are combined in a petri dish to enable fertilization. Once an egg is successfully fertilized, the resulting embryo is gently placed into the female’s uterus, paving the way for its development into a fetus and ultimately a baby. Bedaya Hospital is proud of its exceptional IVF success rates for both fresh and frozen cycles since the nineties, standing as a beacon of hope for countless couples in Egypt and the Middle East.
IVF is recommended for those facing various fertility challenges, including:
- Male infertility issues: For men dealing with fertility issues due to low sperm count, abnormal morphology, or decreased motility, IVF offers a viable solution. Our laboratory technique enables the selection and separation of healthy sperm from the overall sample.
- Age-related fertility decrease: Women above the age of 36 who have been unsuccessful in conceiving for over a year may benefit from IVF. As the quality and regularity of ovulation tend to decrease after 35, medication to stimulate egg production can help yield several high-quality eggs for the procedure.
- Polycystic Ovarian Syndrome (PCOS): Women with PCOS often face irregular ovulation, leading to delayed pregnancy. IVF, in combination with ovulation-inducing medication, has shown promising results in improving pregnancy rates.
- Fallopian tube damage or blockage: By facilitating fertilization outside the body, IVF bypasses issues related to the fallopian tubes.
- Unexplained infertility: IVF can offer a hopeful alternative for those facing infertility without a clear cause.
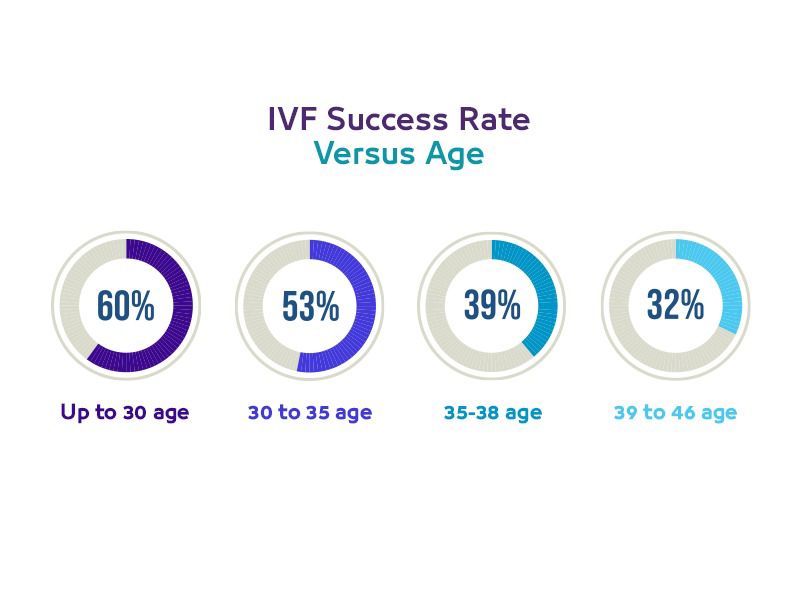
The effectiveness of your IVF journey hinges upon numerous factors, including age and specific infertility causes. Following a thorough evaluation, we advise couples on their chances of achieving a successful pregnancy and whether IVF is a suitable choice. Age significantly influences the success of IVF; hence, some of the highest success rates at Bedaya are noted among couples aged 26–35 years, though we still maintain high success rates for those over the age of 40.
IVF involves the administration of hormones to stimulate the female patient's ovaries to produce multiple follicles, tracked through ultrasound sonography and hormone-specific blood tests. Once mature, the eggs within these follicles are harvested, fertilized with the partner's sperm in our laboratory, and the resulting embryos are carefully transferred back into the uterus. We use multiple embryos for transfer to maximize implantation chances after consultation with the patient.
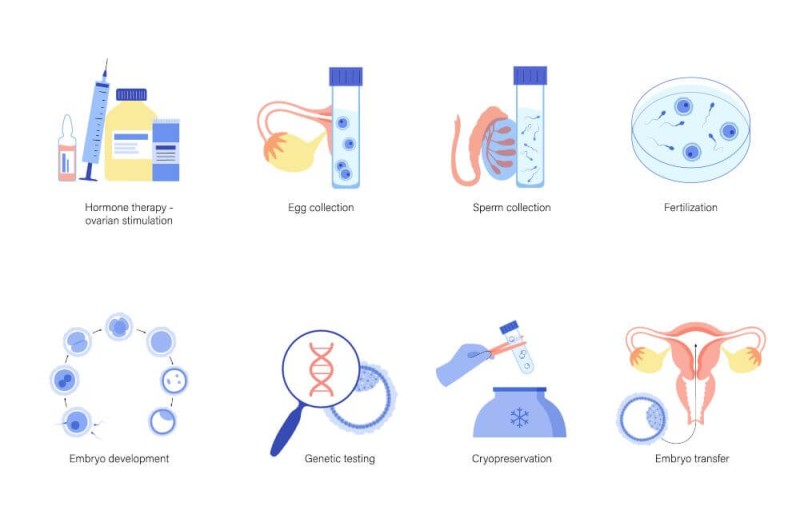
Any remaining, good quality embryos not used in the initial cycle are frozen for future use. These frozen embryos can later be utilized in a frozen cycle, providing an additional opportunity for conception without undergoing a full IVF procedure again.
Majority of our infertility cases are addressed through IVF and ICSI, delivering successful outcomes and happiness to numerous couples who had nearly lost hope. Our hospital is staffed by a dedicated team of highly experienced doctors and professors who excel at diagnosing and treating even the most complex cases.
We attribute our high IVF success rates to our advanced techniques, cutting-edge equipment, and the minor procedures that enhance success rates, such as laser-assisted hatching for IVF and ICSI embryos.
Your IVF journey with us begins with a comprehensive diagnosis by some of the Middle East's top medical professionals. Each IVF procedure is customized to be time-efficient, minimally invasive, and as stress-free as possible. Our state-of-the-art incubators ensure the optimum artificial environment for your embryos, meticulously maintained by our highly skilled embryology team.
We empathize with the emotional, physical, and financial strain of IVF, and we're here to provide support every step of the way. We urge couples above the age of 35 who have been trying to conceive for over a year to seek help without delay. Starting your IVF journey earlier can positively influence success rates. With Bedaya Hospital's internationally recognized high success rates, you can embark on your path to parenthood with trust and confidence. We have helped thousands of families globally fulfill their dreams of starting a family.
the couples have declared that they have visited a lot of fertility centers for IVF and ICSI back in 2011 but with zero results. The 44 years old Fawzy and his wife Awatif with 33 years old were struggling for 16 years to have babies, and they didn’t hesitate to go to Bedaya hospital after hearing about its huge reputation and successful Assisted reproductive techniques. Under the supervision of our medical team, the couple had the procedure in 2016 and was incredibly successful.

