 Book Now
Book Now
2 Ahmed Elmlihy St. from Venny Square, Dokki, Giza, Egypt

Home | Services | Hysteroscopy
Released at:Oct, 12 2023 •
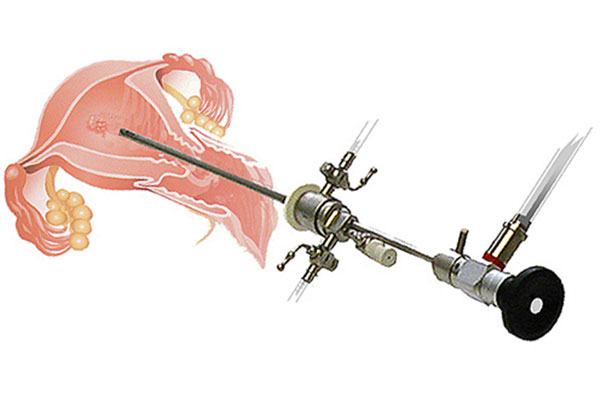
Hysteroscopy is a procedure that allows the treating doctor to look directly into the uterus through the cervix with a tool called a hysteroscope. This is a thin tube with light that is inserted into the vagina goes through the cervix and up to the uterus. Any abnormalities in the cervix or inside the uterus can be seen and usually simultaneously treated by a hysteroscopy surgery. The most common indications for a hysteroscopy procedure are menometrorrhagia (abnormal uterine bleeding), infertility, suspected Mullerian abnormalities, removal of foreign body (polyp, fibroma), confirming something seen on ultrasound or in other tests.
The doctor inserts the tube through the vagina and cervix all the way to the uterus, after that the doctor pumps carbon dioxide or saline to expand the uterus, this way the entire cavity can be seen, and possible minor adhesions parted.
The duration of this hysteroscopy procedure generally ranges from five minutes to about an hour, depending on the diagnosis endoscopically made and the possible hysteroscopy surgery steps of treatment.
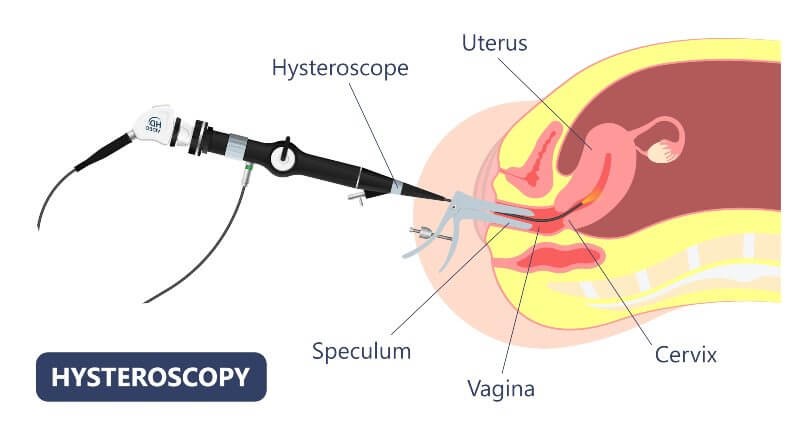
The doctor uses a hysteroscopy procedure to diagnose the following uterine conditions:
In cases of Menometrorrhagia or the abnormal loss of blood a hysteroscopy procedure can be done to find out the reasons for the bleeding and sometimes at the same time treat it by hysteroscope surgery. Bleeding can occur in cases of benign tumors, malignant tumors and polyps. According to size, type and the degree to which any of the above disturb the endometrium lining the gynecologist will decide if they can be treated while he is doing the hysteroscopy procedure. In cases that have menometrorrhagia and infertility or recurrent abortion sometimes the simple removal of small polyps or benign tumors and evening out the endometrium lining through a hysteroscopy surgery makes all the difference.
During a Hysteroscopy polyps, fibroids and tumors up to a certain size can be removed through a hysteroscopy surgery, holding into account that they do not seem suspicious of being malignant (cancerous).
There are different types and degrees of uterine malformations that could affect a woman’s fertility. Recurrent and incomplete pregnancies could be caused by a uterine septum (barrier) in the uterus this malformation can be removed surgically under guidance of a hysteroscope and its tools.
Ashermann syndrome among other reasons can cause uterine adhesions; this means that the uterine walls are at different points or completely stuck to one another. Uterine adhesions are usually accompanied by painful irregular menstruations but could also lead to nonexistent menstrual cycles resulting in infertility or recurrent abortions. A hysteroscopy procedure could help your doctor visualize and accordingly treat them through hysteroscopy surgery
Diagnostic hysteroscopies are done to accurately diagnose something that by medical history, symptoms or after an ultrasound sonography is suspected. It can also be done to evaluate the cervix, endometrium lining, uterine cavity and fallopian tube orifices in cases of infertility or recurrent abortion. The doctor inserts a camera through the vagina, cervix and into the uterine cavity while evaluating what he sees on a screen.
A therapeutic or (operative) hysteroscopy is a hysteroscopy where not only the cervix, uterine cavity and fallopian tube ostia have been evaluated but where during the evaluation a deviation was found and operatively treated through hysteroscopy surgery.
A hysteroscopy procedure like discussed earlier is a procedure that can both diagnose and treat patients. In IVF it is important to determine the state of the endometrium lining making sure there are no polyps or irregularities in the cavity in which the embryos will be returned. A small scratch in the endometrium has also showed to increase the implantation rates after Embryo Transfer (ET). Your doctor will determine whether it is useful in your case to do this and when. Many women fear doing a hysteroscopy and worry about pain, recovery time and complications. It must be said that this procedure is officially called an office hysteroscopy and could in most cases be done in the clinic without anesthesia.
A hysteroscopy procedure has many advantages, it is a diagnostic and operative tool of treatment that is less invasive, requires less time in the hospital and has less complications than other methods. It has also proven to considerably increase pregnancy rates in IVF and ICSI cycles in general not only if it removes a polyp or fibroid that could work as an Intra Uterine Device (IUD).
Undergoing a hysteroscopy procedure usually does not disturb your menstrual cycle and your regular menstruation should come 3-5 weeks after your procedure, sometimes there will be some minor vaginal bleeding or spotting after undergoing the hysteroscopy which is normal. The doctor usually recommends doing the hysteroscopy procedure the first days after your menstruation so the cervical entrance is still open, but he can decide otherwise if he sees it fit.
Undergoing a hysteroscopy usually takes from 15 min to an hour depending on whether you need treatment or not. If the hysteroscopy was done without anesthesia the recovery time is usually 15 min. If anesthesia was recommended by your physician, the recovery time usually takes an hour or two and you will remain under observation until the anesthetic drug has worn out.
After a hysteroscopy procedure, you may notice some disturbing symptoms such as:
For her

For her
This young Egyptian couple stepped in Bedaya hospital with positive energy, and deep faith of having a child. Indeed, success was their ally from the first time, and Shaima was enabled to give birth to a healthy, handsome child with the help of our medical staff.

